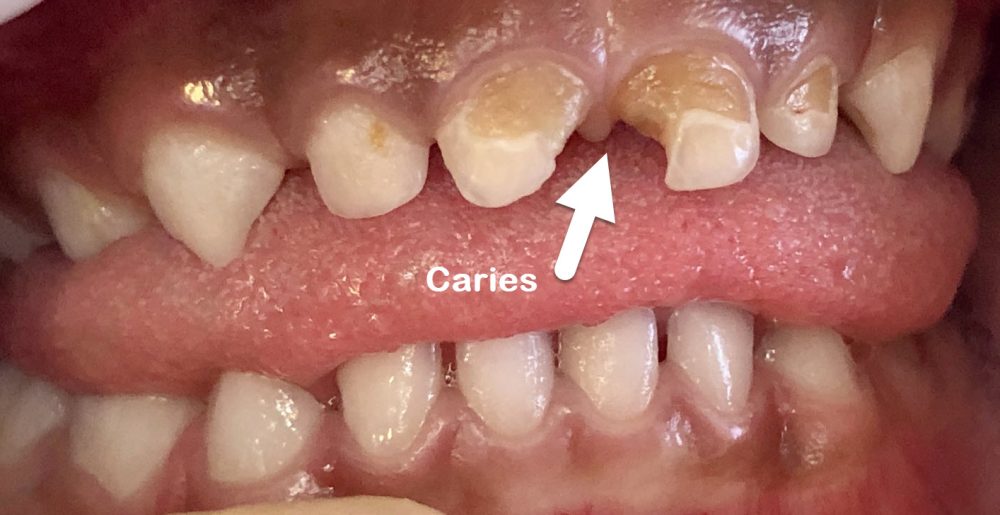
Dental caries remains the most prevalent chronic disease worldwide. A white spot lesion (WSL) is the outcome of enamel demineralisation and is characterised by a change in colour (brown or white) and/or glossiness prior to the loss of surface integrity.
Since treating a WSL is much less challenging compared to once it is cavitated, the main goal in modern dentistry is the early detection, protection, and remineralisation of incipient lesions.
In recent years there has been a dramatic shift away from traditional invasive treatment approaches, because of the ‘Repeat Restoration Cycle’, and a move to a more preventative approach, namely non-invasion or microinvasion. Resin infiltration is a novel micro-invasive technology that aims to bridge the gap between preventive and restorative therapies.
It is a low viscosity-resin intended primarily for the management of smooth surface and proximal uncavitated lesions. It works by permanently occluding porous enamel by capillary action, thereby establishing a barrier against acids and dissolved materials that would otherwise promote cavitation and lesion progression. It has an additional positive effect of camouflaging aesthetically unsightly WSLs on facial surfaces. There are many laboratory and clinical studies in the literature that show promising results for resin infiltration. However, there is still uncertainty within the dental profession regarding its efficacy in treating uncavitated enamel lesions on (i) proximal, occlusal, and facial/ lingual surfaces and (ii) primary and permanent teeth.
This review aims to assess this. A database search was conducted in August 2021, from which 14 studies were deemed suitable. Overall, it was found that while statistically significant data exists in support of resin infiltration, it still bears many practical limitations that make it currently questionable for its intended mode of treatment. Instead, it is implemented as a successful treatment option for its vestibular cosmetic action on smooth surface WSL. Further experimental studies are needed to optimise resins and infiltration behaviour and thus assist in customised clinical decision making.
Dental caries remains the most prevalent chronic disease worldwide, and its sequelae continue to pose a significant health burden for a diverse range of populations. A 2020 Delphi Consensus emphasises that dental caries is not an occasional cycle of cavitation but a “biofilm-mediated, diet modulated, multifactorial, non-communicable, dynamic disease resulting in net mineral loss of dental hard tissues”.
A white spot lesion (WSL) is the outcome of enamel demineralisation and is the first clinical sign of caries. Also referred to as an incipient, uncavitated or early enamel lesion, it is characterised by a change in colour (brown or white) and glossiness before the loss of surface integrity 3. Once cavitated, management can prove challenging because deeply entrenched bacterial biofilms must be removed while preserving tooth structure and pulpal vitality. Whereas WSLs can reverse
and remineralise relatively quickly as a result of their pseudo-intact surface overlying the lesion. Therefore, detection, diagnosis, and treatment of demineralised but uncavitated caries lesions would be significantly beneficial in offering a conservative alternative to restorative care once lesions become cavitated.
In recent years, the departure from the traditional restorative treatment approach and a move to minimally invasive dentistry (MID) can be supported by a phenomenon known as the ‘Repeat Restoration Cycle’. In essence, they explain that once a virgin tooth has been subject to contact with a bur, the original anatomy, strength, and aesthetics are lost forever, and as a result of clinical failure, a continuum of replacement dentistry will proceed, with repeatedly more extensive restorations, more significant hard tissue loss and ultimately extraction.

The goal of MID is to avoid these long-term restorative needs and costs and ensure teeth are kept functional for life. Greater attention has been devoted to non-invasive and micro-invasive treatment, including remineralisation of lesions with fluoride or therapeutics sealants. Another such nonrestorative caries control (NRCC) measure is resin infiltration.
Resin infiltration is a novel micro-invasive technology that aims to bridge the gap between preventive and restorative therapies. It was first introduced by Robinson et al. in 1976, who attempted to arrest carious lesions by infiltration with resorcinol-formaldehyde resins.
This material was deemed clinically unacceptable due to its toxicity. However, the concept of infiltration has since been modified and commercially developed in Germany into which is now known as ICON® (DMG, Hamburg, Germany). It is marketed as a low-density, low-viscosity, light-curing, methacrylate-based resin matrix, intended primarily to manage smooth surface and proximal uncavitated lesions. It works by permanently occluding porous enamel by capillary action, thereby establishing a barrier against acids and dissolved materials that would otherwise promote cavitation and lesion progression. It has an additional positive effect of camouflaging aesthetically unsightly WSLs on facial surfaces. Figure 1 breaks down the steps involved in infiltration application.
Many laboratory and clinical studies in the literature show promising results for resin infiltration, from in situ studies on artificial caries of bovine teeth, to in vitro and in vivo experiments on human teeth of both adults and children. However, it is essential to note that the authors, Paris et al. are inventors of various patents for ICON ®, stating that they receive royalties from the manufacturer. Furthermore, Ekstrand et al. and Alkilzy et al. disclosed that they were financially supported for the relevant research from the DMG Dental-Material GmbH (Hamburg, Germany). Although no conclusions are being drawn to discredit their findings, it calls for more future studies on resin infiltration by authors who do not have a financial interest in the material.
Therefore, the objective of this essay is to critically appraise the current evidence on resin infiltration for the clinical management of uncavitated caries lesions. This will be done by exploring the comparative effectiveness of resin infiltration over non-invasive, invasive and other micro-invasive therapies on (i) facial, proximal and occlusal surfaces and (ii) primary and permanent teeth. An uncavitated enamel carious lesion is represented as either up until an ICDAS 2 (distinct visual changes in enamel opacity) or a maximum radiological extension into the inner half of enamel.
Electronic searches were conducted in August 2021, covering Pubmed, EMBASE and Cochrane Library. Additionally, literature was identified from the reference list of selected articles. 14 studies altogether were deemed suitable for inclusion in this review. Data for 13 of them were extracted and tabulated in a standardised manner. Ultimately, this analysis would guide us in determining whether the resin infiltration technique is a promising micro-invasive approach that could be implemented in clinical practice and thus complement the concept of MID.
Biofilm control via non-invasive treatment includes mechanical removal of plaque (brushing, interdental cleaning), antibacterial treatment (e.g., chlorhexidine varnishes or mouth rinses) or remineralisation therapy (e.g. sodium fluoride [NaF] varnish). Since sufficient patient compliance combined with a low-cariogenic diet are generally required for non-invasive approaches to be successful, resin infiltration can be regarded as a favourable alternative.
Numerous clinical investigations reveal that combining resin infiltration with fluoride varnish demonstrated a superior reduction in lesion progression than varnish alone, notably proximal uncavitated lesions showed a five times greater chance of arrest when treated with resin infiltration and 5% NaF varnish. A recent study further claims that, unlike fluoride, resin infiltration provides mechanical stabilisation to demineralised enamel. With the added benefit of single visit treatment, rather than periodic visits as in the case of non-invasive therapies, resin infiltration, seems like an ideal alternative.
However, a significant disadvantage of resin infiltration is the need for surface conditioning with 15% HCI. HCI is necessary for optimal infiltration, but with a penetration depth of 58μm, it subsequently destroys the surface integrity of the enamel.
If an intensely eroded enamel surface is insufficiently infiltrated, this can cause lesions progression and consequent secondary caries. A second disadvantage is its need for isolation due to (i) its extreme hydrophobicity and (ii) HCI toxicity that may cause soft tissue irritation or ulceration. Therefore, a rubber dam is necessary, but the lesion area also needs to be pretreated with alcohol (Icon-Dry) to remove water from inside the pores. Lastly, infiltration is far more costly than fluoride treatment.
The conventional ‘drill and fill ‘ approach requires the destruction of a substantial amount of sound tooth structure and are especially contraindicated for proximal lesions of primary teeth.
Particularly in uncavitated lesions, substituting the drill with resin infiltration would prove beneficial in preserving hard tissue, reducing the risk of post-operative sensitivity or adverse pulpal reactions, minimising patient discomfort or anxiety and most importantly, is less likely to perpetuate the ‘Repeat Restoration Cycle’. Despite being more costly than fluoride treatment, compared to invasive action, it is economical for both the patient and the dentist. The availability of electrical supplies does not limit access. Nevertheless, not all cases are recommended for resin infiltration. Manoharan et al. report that teeth with brown discolouration are not good candidates for resin infiltration. Rather than masking the brown colour, they may accentuate it and yield a worse aesthetic outcome. They indicate that microabrasion or conventional restorations may be better options for treating such lesions. Therefore, caution should be taken for case selection.
Apart from resin infiltration, fissure sealing for children in Brisbane is another form of microinvasive treatment. This technique maintains a diffusion barrier superficially on the enamel surface rather than inside the lesion body. Another key difference is that resin sealants use 37% phosphoric acid (H3PQ4) instead of 15% HCI as a form of pre-treatment or, in the case of GIC sealants, no acid-etching is required. Paris et al. report that a significantly deeper penetration was achieved by resin infiltration ( 41 % ) into ICDAS 2 fissure lesions instead of fissure sealing (5% ).
They credit this advantage to (i) the infiltrant’s higher penetration coefficient (147m/s RI vs 4cm/s FS); (ii) longer application time, and (iii) more intense erosion of the surface layer as achieved by HCI ( 15% for 120 seconds) as opposed to H3PQ4 (37% for 60 seconds). However, in the same study, they discovered that while sealants filled most fissures, the infiltrant did not. The presence of residual biofilm and calculus after surface conditioning could be responsible for this contradiction, implying that even etching with HCI may not be sufficient in cleaning demineralised surfaces.
An earlier study from the same authors reinforces that HCI may contribute to incomplete surface layer erosion. However, from a biological point of View, HCI etching can significantly reduce enamel thickness compared to H3PQ4, and if an eroded surface is not correctly infiltrated, lesion progression can be facilitated. Interestingly, Neuhaus et al. raise the question of whether full penetration of an infiltrant is vital and if a firm surface seal (i.e. a fissure seal) is adequate in controlling lesion progression. Compared to infiltrants, sealants are more likely to produce sealant margins if excess material is not removed and subsequently promote the formation of secondary caries and periodontal inflammation.
Another critical clinical benefit of infiltration, in contrast to sealants, is that it can be performed in a single visit because they do not require special orthodontic separation placed a few days prior since minimal separation from available wedges and applicator foils are sufficient. In their Cochrane review, Dorri et al. reported a net trend to find resin infiltration slightly more efficacious than resin sealant. Nevertheless, the previous limitations suggest that resin infiltration requires further optimisation, and for this to occur, more standardised experiments are necessary.
While this therapy appears to complement the concept of minimal intervention dentistry, there is the need to mention some further limitations that may affect its success in practice: increased surface roughness, polymerisation shrinkage, non-homogenous filling and the conflicting evidence regarding surface microhardness.
Increased surface roughness In a recent study by Gurdogan et al., which evaluates the properties of resin infiltration at nano-scale, ICON ® samples was found to have a higher surface roughness than sound enamel. Two other studies found similar data, specifically that the infiltration application caused a surface roughness higher than 200nm and thus could contribute to plaque accumulation.
Polymerisation shrinkage: Deep lesions can be associated with polymerisation shrinkage of the resin infiltrant and lead to marginal leakage, one of the main reasons for secondary caries. To compensate for this shrinkage, manufacturer guidelines advise applying the infiltrant twice, infers prolonged chair-time, greater opportunity for error and decreases patient acceptance.
Nonhomogeneous filling: Furthermore, resin infiltration can display non-homogenous filling and be sub~tantially unpredictable. Deeper lesions have a reduced chance of achieving complete filling. Similarly, active lesions are more deeply penetrated than inactive lesions, and if both types exist simultaneously on a given surface, a non-uniform filling can be expected.
The presence of air bubbles can also contribute to impeding the flow of infiltrant 15. Finally, a similar outcome can be associated with the pit of the fissure system due to its extensive network of cusps and isthmuses. Therefore, resin infiltration is not indicated for use on occlusal surfaces and considering its unpredictable nature, further investigation needs to be undertaken on whether it is an efficacious method for treating uncavitated lesions on any surface, for that matter.
Conflicting evidence concerning surface microhardness Studies shows differing results related to microhardness following resin infiltration. Paris et al. reported that significantly higher microhardness values were observed on infiltrated bovine enamel in comparison to healthy enamel. In contrast, two studies found no significant difference in microhardness values between ICON ® and healthy enamel. Furthermore, Following an acid challenge, fluoridated teeth exhibited no reduction in microhardness, while groups treated with resin infiltration had decreased values. They attribute this to a combination of insufficient infiltration and resin shrinkage, thus suggesting that lesions are still susceptible to demineralisation even after resin infiltration.

Is resin infiltration efficacious in treating proximal uncavitated enamel lesions? The prevalence of proximal caries has undergone only a meagre decline in comparison to other surfaces caries, compromising more than half of all reported caries. Relating toproximal lesions, this review identified studies, all of which reported a statistically significant reduction in lesion progression in resin infiltrant groups compared with control groups (no intervention, fluoride treatment and oral hygiene instructions).
These findings align with the management guidelines published by two breakthrough systematic reviews. They confirm that when resin infiltration is used alone, there was a two times greater chance of arrest or reversal of interproximal uncavitated lesion and five times greater chance when used adjunctly with 5% NaF varnish. Despite this, Slayton et al. prioritise 5% NaF varnish upon accounting for all factors before resin infiltration. This underlines that although resin infiltration appears superior in theory, there is a lack of long-term clinical experience, and it may not prove pragmatic for reasons such as technicality, unpredictability, and cost. Therefore, at current, the use of 5% NaF varnish is preferred to resin infiltration (+/- 5% NaF varnish) for treating uncavitated proximal lesions.
Is resin infiltration efficacious in treating occlusal uncavitated enamel lesions? 2 studies focusing on occlusal non cavitated lesions reported that infiltration was more effective than NaF varnish and fissure sealing, respectively. However, the aforementioned limitations relating to the use of infiltration on occlusal surfaces, such as the unfavourable pit and fissure morphology, impaired filling and presence of air bubbles must not be overlooked.
Accordingly, Slayton et al. rank resin infiltration (plus 5% NaF varnish) fifth in their list of guidelines for managing occlusal non-cavitated lesions while endorsing sealant in conjunction with 5% NaF varnish as the current gold standard. Resin infiltration is not suitable for use on occlusal surfaces, and further development and research is imperative.
Is resin infiltration efficacious in treating facial/ lingual uncavitated enamel lesions? The prevalence of WSLs on smooth surfaces is relatively high, ranging from 24 to 70% in primary teeth. Although both included clinical trials report resin infiltration to be more efficacious in preventing lesion progression than fluoride varnish, Slayton et al. and Urquhart et a l. does not endorse the former as an ideal regiment for arresting uncavitated smooth surface lesions. Instead, they recommend 5% NaF varnish or 1.23% APF gel as the recommended treatment option for facial/ lingual uncavitated lesions on permanent and primary teeth.
This evident disparity between findings suggests that more research on resin infiltration for smooth surface lesions are imperative, especially as high levels of fluoride have been warned against treating WSLs on labial surfaces since they arrest a lesion through rapid remineralisation rather than completely repairing it.
The vestibular aesthetic effect of resin infiltration: Interestingly, Brisbane paediatric dentists commonly use resin infiltration on smooth surfaces for its vestibular cosmetic advantage: masking WSLs. Infiltration application can improve the colour because its optical properties are similar to that of natural enamel. In their clinical study, Cocco et al. illustrate that fluorosis spots lost their whitish appearance after infiltration. Likewise, Kim et al. specify that instantaneous masking effects were seen in some but not all infiltrated teeth with developmental defect enamel and post-orthodontic decalcification. There is an evident need for clinical studies to test whether resin infiltration maintains these aesthetic results in the long term.
Is there a difference in infiltration effect between primary and permanent teeth?
Very few studies have been undertaken that test how permanent and primary lesions differ by their degree of resin infiltration. It is well known that primary enamel has a more significant diffusion coefficient than permanent enamel, indicating it is less mineralised, more porous and aprismatic. Therefore, it can be expected that penetration of a resin infiltrant will be deeper and faster than permanent teeth. This phenomenon is reflected by Paris et al., who exhibited that uncavitted proximal lesions in primary molars were deeply infiltrated after 1 minute of application, while previous studies demonstrated that complete infiltration in permanent teeth was only obtained after 3 to 5 minutes of application. The consensus amongst dentists is that resin infiltration is technique sensitive and may not be appropriate for uncooperative children, even if the application time is only 1 minute instead of 3 or 5 minutes. It is noteworthy to point out that the progression rate of proximal caries in primary teeth is significantly higher than molar teeth due to their thinner and less mineralised proximal walls. This means that resin infiltration must be performed with extra diligence in primary teeth, absent of any voids or additional material, to ensure no secondary caries ensues. Moreover, since proximal surfaces are the most common caries site for primary teeth, performing substandard resin infiltrations would measure a high failure rate.
Therefore, the question arises, can resin infiltration be considered a significant addition to a dentists’ treatment armamentarium for the management of uncavitated enamel lesions? Based on laboratory and clinical evidence, it appears it should arrest lesion progression in enamel lesions, even more so than fissure sealing and fluoride varnish. However, as a dentist, it is prudent to assess a novel technology holistically rather than quantitatively.
Therefore, upon considering the limitations discussed in this review, resin infiltration should only be implemented to improve the clinical appearance of WSL on smooth surfaces. Furthermore, treatment should be tailored to the patient based on their caries risk, degree of compliance, age, and other critical factors. With further improvements, it may be possible to use resin infiltration as a preventative and therapeutic agent, rather than simply a cosmetic one. For this to occur, further standardised experiments need to be designed to smooth out uncertainty regarding treatment effects and assist in clinical decision making.